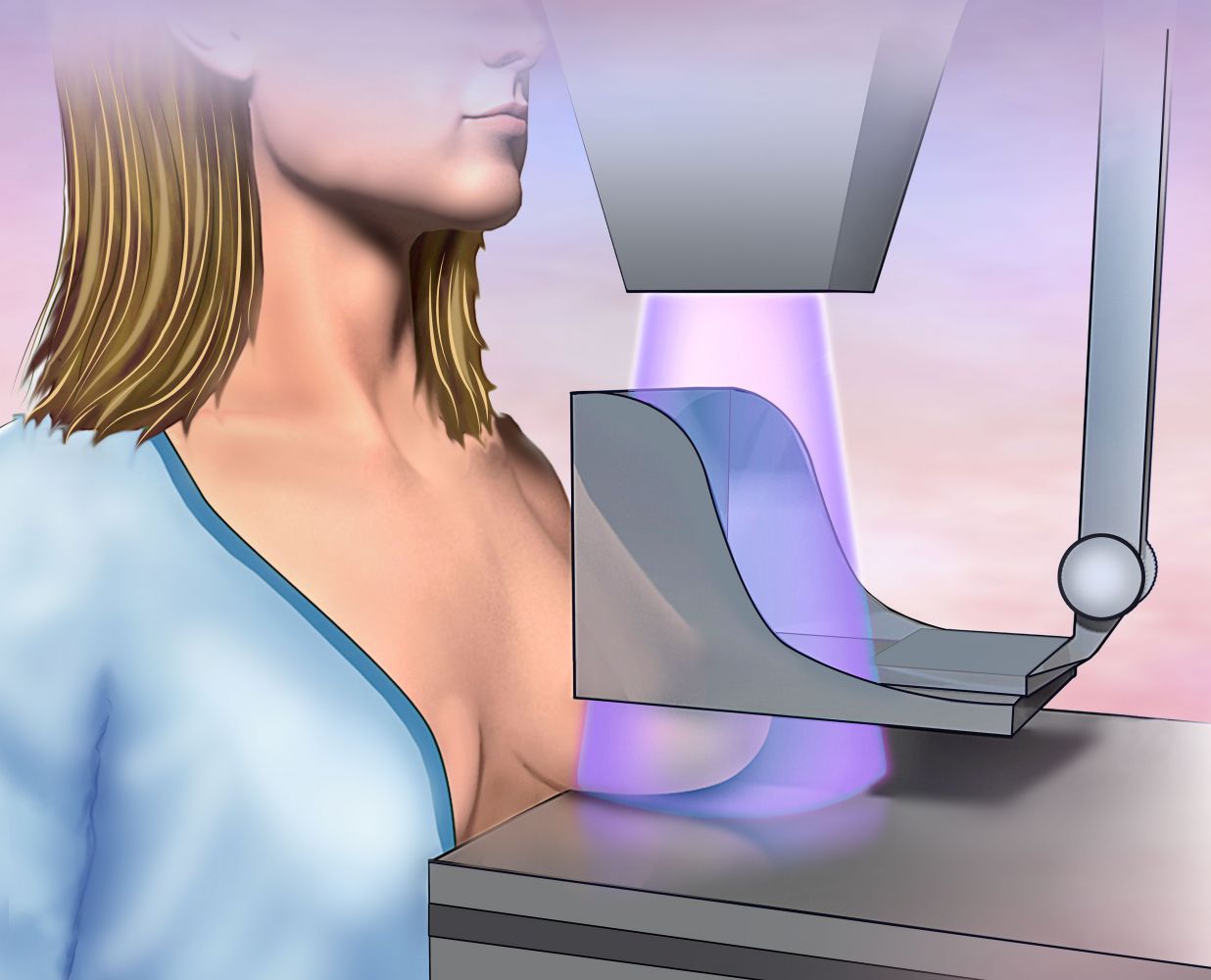
In 1972 the American Cancer Society (ACS) together with the National Cancer Institute (NCI) developed Breast Cancer Detection Demonstration Project, aimed to perform X-ray mammography breast cancer screening for more than quarter of a million of American women.
Since then, X-ray mammography has become not only the main screening method but also the ‘gold’ standard in diagnostics. It is important to distinguish between screening tests and early diagnostics. Early diagnostics implies early detection of tumours in patients with symptoms. The screening test means early detection of tumours in patients without symptoms (1). Nowadays, X-ray mammography is used for screening as a method of early diagnostics of breast cancer. However, used as a screening method, X-ray mammography has its limitations and drawbacks. We’ll name some problems of the main screening method.Age. Women aged below 40 usually do not undergo breast cancer screening since sensitivity of mammography is low in this population due to high density of breast tissue (2). It was discovered that mammographic screening under the age of 50 is not only less effective than in the elder age but is also related to higher radiation risks (3). Expanding the screening age range below the age of 40 is undesirable since it will lead to the increase of patients’ radiation exposure. Age limitations for X-ray mammography are closely related to the breast cancer morbidity.
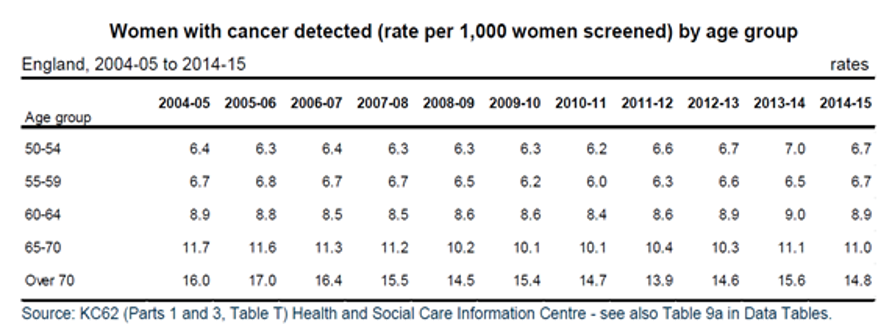
Morbidity. According to the data of Health & Social Care Information Centre (England, 2016), despite screening programmes, breast cancer morbidity does not decrease, it remained on the same level for all age groups for 10 years since 2004-2005 till 2014-15 (Table 4). For the sake of solving the problem of morbidity it would seem only natural to shift the screening framework down along the age scale. However, age limitations do not allow for that.
Operational characteristics (sensitivity and specificity). Screening survey is a survey with low prevalence. As a rule, a low-prevalence survey is a preventive checkup. Screening survey is characterized by unrestricted sampling, usually estimated in many thousands; by low prevalence; standardized procedure; significant predominance of healthy patients over patients with pathologies; impossibility to use a reference method and histological verification of diagnosis due to a large number of healthy patients; significant predominance of early stage of disease among the affected patients; impossibility to apply operational characteristics, i.e. sensitivity and specificity. It is impossible to get operational characteristics and incidence data from the screening survey data. Operational characteristics can be received from the examination of patients with symptoms.
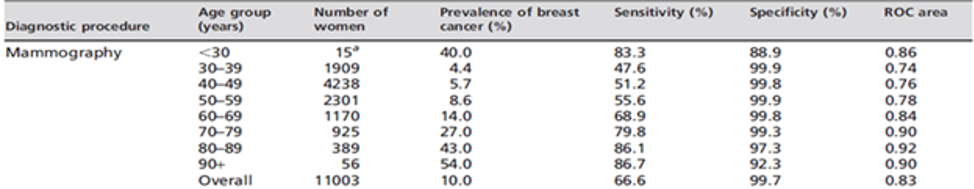
The table shows operational characteristics of X-ray mammography received during a 6-year period from a large group of patients with symptoms (5).
Sensitivity of X-ray mammography used for breast cancer diagnostics above 80%, which would satisfy screening requirements, is observed only in the 70-79, 80-89 and 90+ age groups.

Screening interval. Screening interval is a period of time between two subsequent screening tests. It is considered that this interval is directly connected with prevalence, dynamics of development of the disease targeted by screening, operational characteristics of the applied methods (1). During calculation of the screening interval, along with these factors, the patient’s radiation exposure should be taken in account. According to the definition of the World Health Organization, screening is a complex, repetitive and continuous procedure and is not a one-time-only action (Principles and Practice of Screening for Disease).
Breast density – Breast cancer is often similar to X-ray density of fibroglandular tissue, which makes it difficult to distinguish these tissue types due to the masking effect of dense glandular tissue (6). It explains the unreliability of X-ray mammography for cancer diagnostics in women with high-density glandular parenchyma, with fibrocystic disease. Women with high mammographic density have higher risk of breast cancer occurrence (7). It has been proved that high mammographic density can be related to quadruple increase of breast cancer risk (8, 9).
Formation of survey or risk group. According to the definition of the World Health Organization “there should be a recognizable latent or early symptomatic stage. The natural history of the condition, including the early stage, should be adequately understood”. Thanks to screening, it becomes possible to form breast cancer risk groups. Since ductal carcinoma takes origin from epithelial cells, areas with fibroglandular tissues and large amount of cells are highly susceptible to the increased epithelial proliferation (10). It is the quantitative estimation of the state of fibroglandular tissue that should be used as the selection criterion allowing to differentiate the norm and the pathology. Patients with the amount of fibroglandular tissue abnormal for their age should become a part of the surveillance group. The existing screening methods do not allow to form breast cancer surveillance groups.
Repetitive examinations. Screening is a dynamic process. Recall of a patient for the screening programme may cause anxiety or serious worries about potential illness, the so called Ulysses syndrome, and lead to repeated radiation exposure (11). In this connection, it is sensible to use safe screening methods that allow for multiple repetitive examinations. Frequency of examinations especially among high-risk group patients and in cases of hormone replacement therapy is chosen on an individual basis depending on the pathology detected.
Radiation exposure. Glandular tissue in the breast is most susceptible to radiation exposure compared to fat, skin and areola since immature cells are more vulnerable to ionizing radiation exposure (12). And since ductal carcinoma takes origin from epithelial cells, it leaves one perplexed why X-ray mammography is used in breast cancer screening programmes. Mammography has increased risks of radiation-induced breast cancer. Supposedly, low radiation dose is riskier compared to higher radiation dose (13, 14).
Rupture risk. The mammography procedure carries a risk of rupture of encapsulated cancer tumour, which may occur during the compression of breast tissue, and it may lead to metastases. Modern mammography equipment uses 42 pounds of pressure (15). It may suffice for the disintegration of capsule and formation of metastases.
Mammography technique. According to the criteria of disease screening, the diagnostic method should be accessible and acceptable for the population (PRINCIPLES AND PRACTICE OF SCREENING FOR DISEASE). Mammography technique can be evaluated through the analysis of the dose applied, the quality and size of the ray, the specific compression of breast. It has been established that the radiation dose and growth of breast cancer incidence are related (16). Direct calculations of radiation dose (mGy) for a specific mammary gland are impossible. The difficulty lies in the knowledge of the structure of a specific mammary gland, which is necessary for the calculation of the conversion ratio. For this reason, an average dose is used, which depends on the thickness of the breast. In modern mammographs the exposition is selected automatically based on the thickness of the compressed breast. Specific compression of the breast is the baseline for a good-quality image. Errors that may occur in the calculation of breast thickness during the compression of breast are related to the compression panel that may get bended and deformed.
These data show the necessity to implement additional effective screening programmes for young women including screening with the application of alternative technology in order to lengthen the pre-clinical detection stage, which would lead to the decrease of breast cancer mortality rate (17). In order to overcome the existing limitations, it is necessary to use modern alternative methods of breast examination that would be equal to the ‘gold’ standard in its effectiveness. Electrical impedance mammography is a diagnostic method satisfying the criteria set by the World Health Organization for screening for diseases. MEIK v.5.6, electrical impedance mammograph developed and manufactured by PKF SIM-technika Ltd., Russia, uses advanced technologies of imaging and processing of electrical impedance images of breast. It is a noninvasive technology of image creation, it uses 3D-tomography system, it is a form of ‘soft-field’ tomography, it applies ‘non-local’ method of tomographic imaging and cross-sectional approach to data collection, it uses back-projection method with vertical and horizontal weighing function, and finally it allows to receive quantitative diagnostic information.
- CANCER SCREENING AND MORTALITY A.A. Barchuk, A.M. Belyaev, A.V. Filochkina, A.I. Arseniev, Anssi Auvinen практическая онкология, Т. 17, №4-2016
- Gabriel and Domchek Breast Cancer Research 2010, 12:212
- Mammographic screening before age 50 years in the UK: comparison of the radiation risks with the mortality benefits.Berrington de González A1, Reeves G. Br J Cancer. 2005 Sep 5;93(5):590-6
- Breast Screening Programme, England. Statistics for 2004-15 Published 24 February 2016. Health & Social Care Information Centre
- Measuring the accuracy of diagnostic imaging in symptomatic breast patients: team and individual performance P BRITTON, J WARWICK, M G WALLIS, S O’KEEFFE, K TAYLOR, R SINNATAMBY, S BARTER, M GASKARTH, S W DUFFY and G C WISHART The British Journal of Radiology, 85 (2012), 415–422
- Leung et al., 2010 Can Breast Magnetic Resonance Imaging Demonstrate Characteristic Finding of Preoperative Ductal Carcinoma in Situ in Taiwanese Woman? Asian Journal of Surgery, Vol. 33, No. 3, pp. 143-149
- Relationship between mammographic density and the risk of breast cancer in Japanese women: a case-control study.Nagao Y, Kawaguchi Y, Sugiyama Y, Saji S, Kashiki Y. Breast Cancer. 2003; 10(3):228-33.
- Boyd et al., 1998 Mammographic Densities and Breast Cancer Risk. Cancer Epidemiology, Biomarkers & Prevention, Vol. 7, pp. 1133-1144;
- Kolb et al., 2002 Comparison of the Performance of Screening Mammography, Physical Examination, and Breast US and Evaluation of Factors that Influence Them: An Analysis of 27,825 Patient Evaluations. Radiology, vol. 225, No. 1, pp. 165-175
- McCormack & Santos et al., 2006 Breast Density and Parenchymal Pattern as Markers of Breast Cancer Risk: A Meta-Analysis. Cancer Epidemiology, Biomarcers & Prevention, Vol. 15, No. 6, pp. 1159-1169
- Leung et al., 2002 Will Screening Mammography in the East Do More Harm Than Good? American Journal of Public Health, Vol. 92, No. 11, pp.1841-1846
- Hammerstein et al., 1979 Absorbed radiation dose in mammography. Radiology, 130, 485-491
- Brenner DJ, Sawant SG, Hande MP, et al. Routine screening mammography: how important is the radiation-risk side of the benefit-risk equation? Int J Radiat Biol. 2002;78:1065-1067.
- Heyes GJ, Mill AJ, Charles MW. Enhanced biological effectiveness of low energy x-rays and implications for the UK breast screening programme. Br J Radiol. 2006;79:195-200.
- Hoekstra P. Quantitive digital thermology: 21st century imaging systems. Paper presented at: OAND Conference; 2001; Hamilton, Ontario
- Hammerstein et al., 1979 Absorbed radiation dose in mammography. Radiology, 130, 485-491
- Son et al., 2006 Changing Patterns in the Clinical Characteristics of Korean Patients with Breast Cancer during the Last 15 years. Archives of Surgery, Vol. 141, No. 2, pp. 155-160